Diabetic foot wounds can be challenging to manage due to the complex interplay of complications that affect circulation, sensation, and immune response. For individuals with diabetes, maintaining foot health is crucial to preventing severe complications, such as ulcers and amputations. Orthopedic treatment plays a vital role in diabetic foot wound care, providing targeted strategies to alleviate pressure, manage infections, and support healing. In this article, we’ll explore various orthopedic treatments that are effective in managing diabetic foot wounds, helping patients maintain their mobility and quality of life.
Understanding Diabetic Foot Wounds
Diabetic foot wounds are ulcers that commonly develop on the soles of the feet due to neuropathy and poor circulation, which are hallmarks of diabetes. These wounds often begin as minor abrasions or sores but can quickly progress into deeper, more severe ulcers if not properly managed. The lack of sensation in the feet due to neuropathy means that many patients may not feel the initial pain, leading to unnoticed injuries. As the wound develops, the skin may break down, exposing underlying tissues. Without appropriate care, these wounds can become infected, resulting in serious complications such as cellulitis, osteomyelitis, or gangrene.
Orthopedic Treatment Approaches
Orthopedic treatments for diabetic foot wounds focus on relieving pressure and providing the appropriate environment for healing. Custom orthotics and shoe modifications are often the first line of defense. Custom orthotics are designed to redistribute pressure evenly across the foot, preventing excessive pressure on any one area that could lead to further ulceration. Properly fitted shoes are also critical; they should provide adequate support, minimize friction, and accommodate foot deformities such as hammertoes and bunions. In addition, offloading techniques are used to reduce pressure on the affected foot. This includes the use of special insoles, cast walkers, or custom foot orthotics to prevent weight from bearing down on the wound area.
Debridement and Wound Care
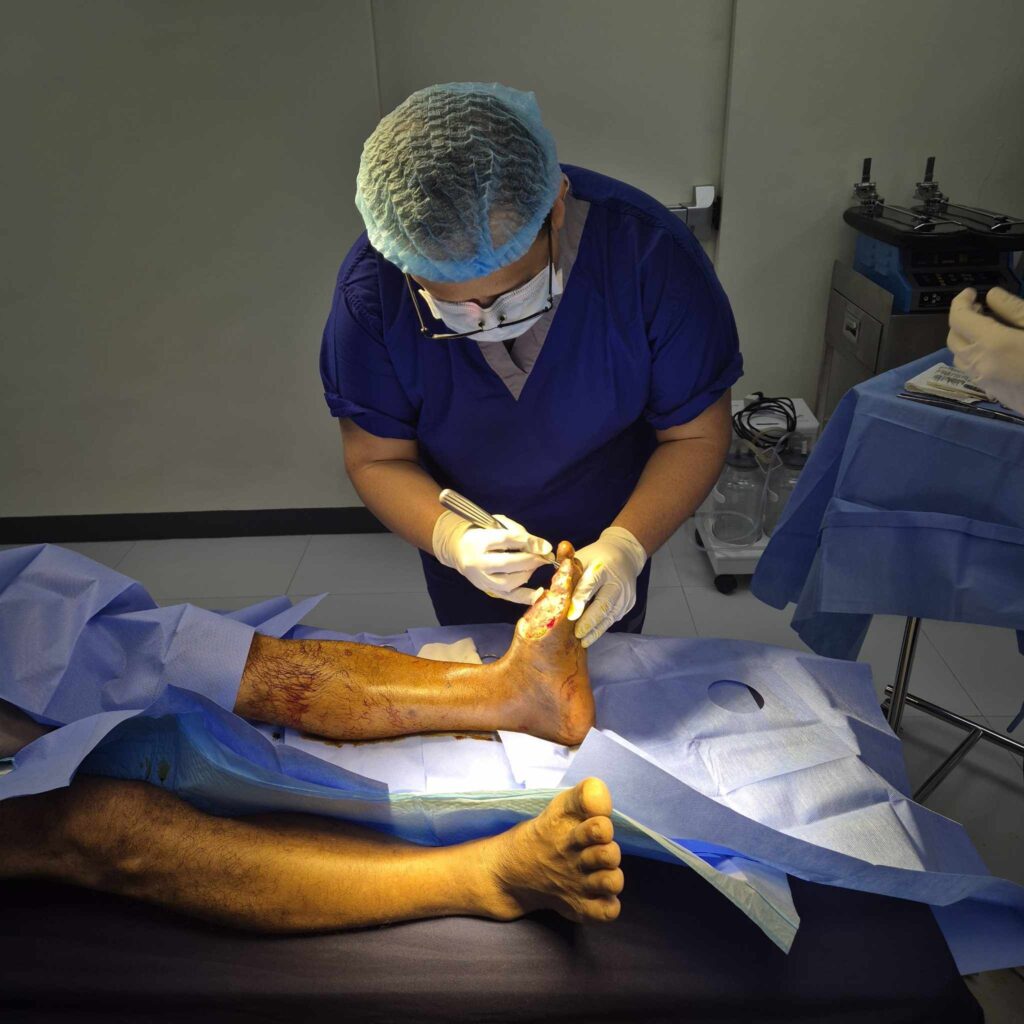
Debridement is a vital procedure in managing diabetic foot wounds. It involves the removal of dead or necrotic tissue from the wound bed, which can act as a barrier to healing. Dead tissue can also harbor bacteria and impede new tissue growth, leading to chronic infections. There are several methods for debridement, including surgical debridement, sharp debridement, enzymatic debridement, and autolytic debridement. The choice of method depends on the wound’s size, depth, and location. Alongside debridement, effective wound care practices are essential. This includes keeping the wound clean, moist, and protected using dressings like hydrocolloids, alginates, or foams, which facilitate a moist environment conducive to healing.
Infection Management
Infection is a major concern in diabetic foot wound care. Signs of infection include increased redness, swelling, warmth, purulent discharge, and pain. Early identification and treatment of infections can prevent serious complications such as sepsis and limb loss. The management of infections often requires the use of topical or oral antibiotics, depending on the severity and type of bacteria present. In some cases, more advanced treatment options, such as hyperbaric oxygen therapy, may be required to enhance oxygen delivery to tissues and promote healing. Regular monitoring by healthcare providers is critical to adjust the treatment as needed and prevent further complications.
Physical Therapy and Rehabilitation
Physical therapy plays a crucial role in diabetic foot wound care, especially for those recovering from ulcer surgery or seeking to prevent future ulcers. Therapeutic exercises are designed to maintain and improve foot and ankle mobility, strengthen the muscles of the feet, and enhance circulation. Techniques such as range-of-motion exercises and resistance training help in preventing muscle atrophy and contractures. Physical therapists may also use modalities like ultrasound or electrical stimulation to improve blood flow and tissue healing. Patients are taught how to perform exercises at home to continue their rehabilitation, ensuring long-term improvement in foot health and reducing the risk of re-ulceration.
Monitoring and Follow-Up
Regular monitoring is vital for diabetic foot wound management. Patients with diabetes should have their feet checked frequently for any changes in color, texture, temperature, and sensation. Healthcare providers will use visual inspections and possibly imaging techniques like ultrasound or MRI to track the wound’s progress. Regular follow-up appointments allow for adjustments in treatment, such as changing dressings or altering pressure relief techniques. During these appointments, patients receive guidance on proper foot care, including how to perform daily foot checks and what to look for in the event of injury. This ongoing management is crucial in preventing the progression of foot ulcers and ensuring effective healing.
Lifestyle Modifications for Prevention
Preventing diabetic foot wounds involves making necessary lifestyle changes that support overall foot health. Maintaining stable blood sugar levels through diet, exercise, and medication is crucial. Blood sugar control is directly linked to reduced risk of foot ulcers, as it helps prevent nerve damage and improves circulation. Patients should be educated on proper foot care, which includes daily foot inspections, avoiding walking barefoot, and using moisturizing creams to prevent dry skin. Shoes should be checked for wear and tear regularly, and patients should avoid tight footwear that can cause blisters and cuts. Educating oneself about diabetes management and foot care can significantly reduce the risk of complications.
FAQ
Q: What are the signs of a diabetic foot wound?
- A: Signs include persistent pain, numbness, changes in skin color, swelling, and the presence of sores or breaks in the skin.
Q: How can I prevent diabetic foot ulcers?
- A: Proper foot care, regular monitoring of blood sugar levels, wearing diabetic shoes, and performing daily foot inspections can help prevent ulcers.
Q: When should I seek medical help for a diabetic foot wound?
- A: If the wound becomes more painful, begins to drain, or if there are signs of infection (redness, warmth, swelling), it’s important to consult a healthcare provider immediately.
Q: Are there any lifestyle changes I should make to help with healing?
- A: Yes, maintaining a healthy diet, exercising regularly, controlling blood sugar levels, and practicing good foot care are essential for wound healing.
Q: What role does blood sugar control play in diabetic foot wound care?
- A: Blood sugar control helps reduce the risk of nerve damage and improves circulation, which is crucial for wound healing and preventing ulcers.